“15 minutes, and I’m already talking to a doctor” – that was the dream of a vast number of patients in the past decade. Now, telemedicine products are turning this dream into reality.
What situations are appropriate to use telemedicine? In the world of healthcare, telemedicine is changing the game by using technology to connect patients and healthcare providers, no matter where they are. This means that even if you live in a remote area, you can still access medical care through virtual visits, messages, and digital platforms.
For patients, the advantages extend beyond convenience. Virtual visits reduce travel time, eliminate geographical constraints, and offer a more flexible healthcare experience. On the provider’s end, telemedicine enhances efficiency, streamlines workflows, and allows for better allocation of resources.
And now, telemedicine is already mainstream, with the main challenge of telemedicine applications lying in weak user engagement and retention.
What are the benefits of telemedicine for patients? Throughout this article, we will delve into these benefits of telemedicine in greater detail and discuss patient engagement methods, shedding light on the positive impact telemedicine has on the healthcare ecosystem.
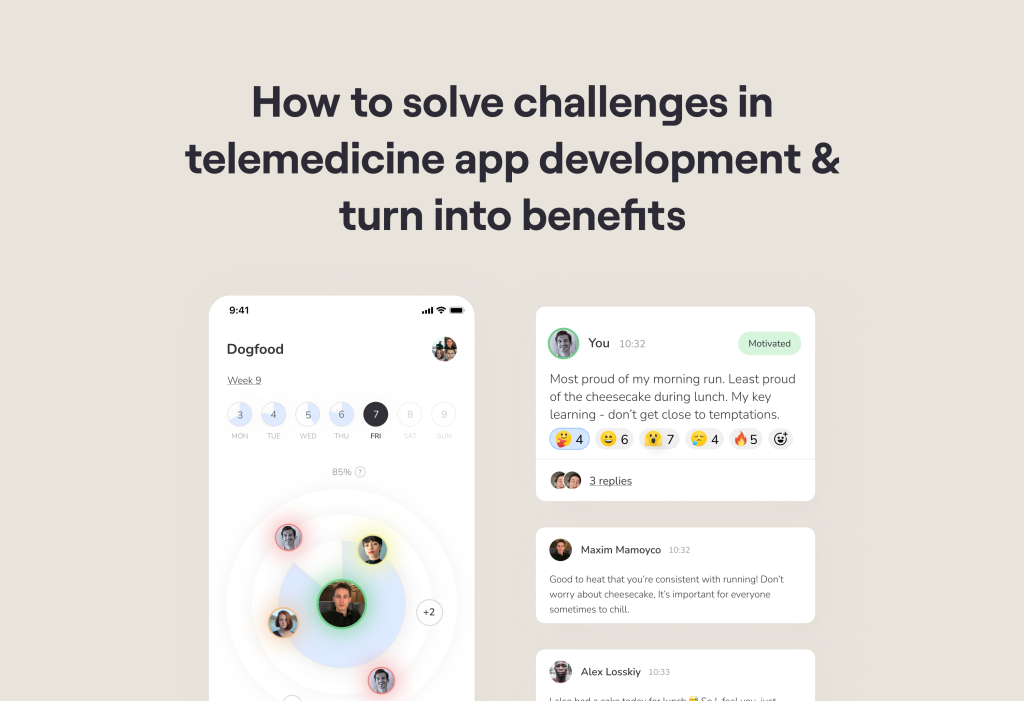
Main challenges in telehealth app development
Who might benefit from telehealth? Of course doctors and patients! But in reality, there are many challenges that we will now consider.
User engagement challenges:
1. Building trust: establishing trust in a virtual healthcare setting is paramount. Users may have concerns about the security of their health data and the reliability of remote consultations. Overcoming these trust barriers requires transparent communication, robust security measures, and user-friendly interfaces.
On how to create a patient trust in a telemedicine app for patients
2. Educating users: telehealth often introduces users to new technologies and processes. Ensuring that users understand how to navigate the app, schedule appointments, and make the most of virtual consultations is a persistent challenge. Clear onboarding processes and user education initiatives are essential.
3. Overcoming technical barriers: this is about limitations of telehealth. Limited access to technology or poor internet connectivity can hinder user engagement. Developers must consider the diverse technical capabilities of their user base and design apps that are inclusive and functional across various devices and network conditions.
Retention challenges:
1. Sustaining user interest: maintaining ongoing user engagement beyond the initial adoption phase is challenging. Developers need strategies to keep users interested, such as providing regular updates, offering additional features, or incorporating gamification elements to incentivize continued app use.
2. Addressing user drop-offs: identifying and addressing points where users disengage or drop off is critical. Analytics and user feedback can help developers pinpoint weaknesses in the user journey and make necessary adjustments to retain users throughout the entire telehealth experience.
3. Communication and follow-up: effective communication is key to retention. Telehealth apps for doctors should facilitate seamless communication between them and patients, including post-appointment follow-ups, medication reminders, and health-related notifications to keep users engaged in their ongoing care.

Patient outcomes challenges:
Who can benefit from telehealth? Of course, patients!
1. Monitoring and tracking health metrics: ensuring accurate and real-time monitoring of patient health metrics is challenging. Developers need to integrate reliable tracking mechanisms, such as wearable device compatibility, to gather continuous health data for better-informed virtual consultations.
2. Ensuring treatment adherence: remote healthcare relies on patients adhering to prescribed treatments and medication plans. Telehealth apps must incorporate features that support and remind users of their treatment regimens, fostering better adherence and improved patient outcomes.
3. Integrating with healthcare ecosystems: seamless integration with existing healthcare systems and electronic health records (EHRs) is essential for comprehensive patient care. Challenges arise in ensuring interoperability and data exchange between telehealth apps for therapists and broader healthcare ecosystems.
We have written a whole book in more detail about how to overcome these challenges.
If you want to delve a bit deeper into this topic, we’ve also created a comprehensive guide on how to boost CX and user engagement:
1. Our best CX (UI/UX) practices to make an app not just used but loved
2. Product strategies to drive retention and engagement
3. Our best Engineering practices to build scalable solutions
4. Tips to ensure compliance with healthcare regulations

Download Free Actionable Insights to Grow your Digital Health app
So what are the benefits of telemedicine for patients and doctors? Advantages of telemedicine are numerous, and we’ll explore them in detail. Telemedicine benefits for patients and benefits of telemedicine for doctors are significant.
1. Accessible and convenient healthcare
One of the key advantages of telemedicine via mobile apps is the increased accessibility to healthcare services. Patients no longer need to endure long travels or wait in crowded waiting rooms; instead, they can connect with healthcare providers from the comfort of their homes using a smartphone and a healthcare app.
For instance, when we were developing a mental health app for our partners at Allbry, we paid special attention to the navigation. We made it resemble WhatsApp on one hand, based on User Tests, and assisted users in getting acquainted with the interface through arrows during onboarding.
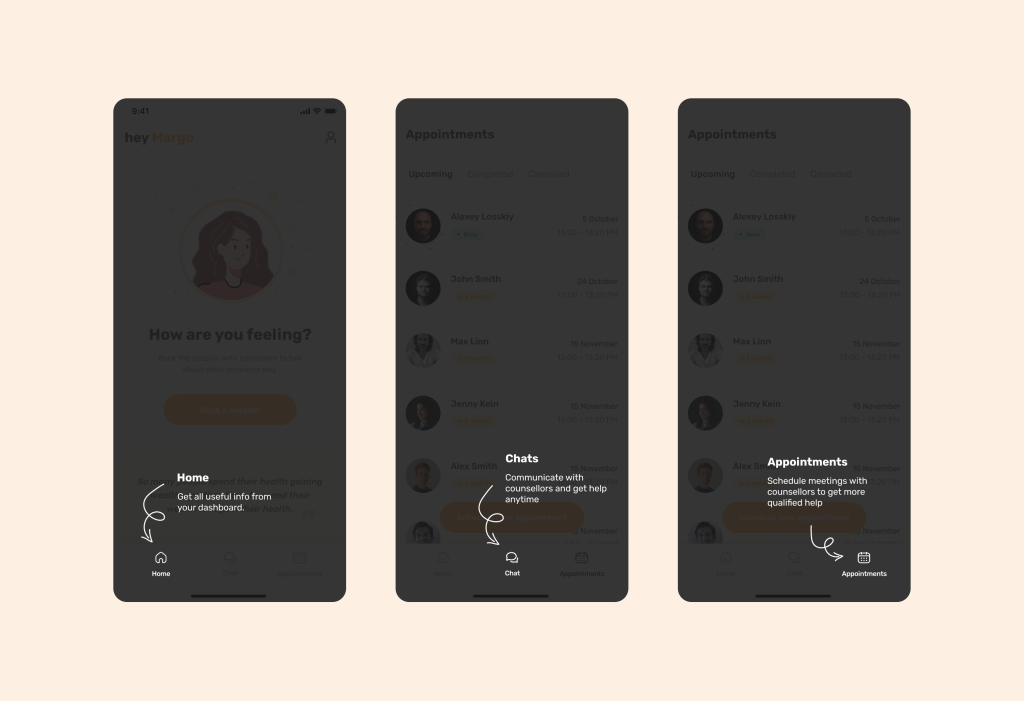
Additionally, we adhered to Haptic Feedback because we wanted users with poor vision to have no difficulties in learning the interface. By incorporating tactile sensations, such as gentle vibrations or touch responses, digital health apps can create a more immersive and engaging user experience.
We implemented vibration for negative scenarios: when an error occurs, the vibration is sharp, which prompts the user to pay attention to what should not be done. On the contrary, a gentle vibration is used (while logging in to the application or performing a task).

Learn how we’ve built telemedicine mental health platform for Swedish startup
In this way, we implemented the telehealth pros and took into account the cons.
2. Broadened geographic reach
Telemedicine benefits for patients include eliminating geographical limitations, enabling patients to consult with specialists located in different cities, states, or even countries through healthcare app development. This expanded reach ensures that patients can access the best care and expertise without being hindered by distance.
A patient in a remote village can receive expert advice from a renowned specialist in a distant city, ensuring optimal care for their condition. So healthcare providers expand their practices.
Moreover, there are more benefits of telemedicine for patients. For example, for our partners at Microshift, we created the option to share the sensations experienced during completed exercises with other individuals, and people actively engaged in communication.
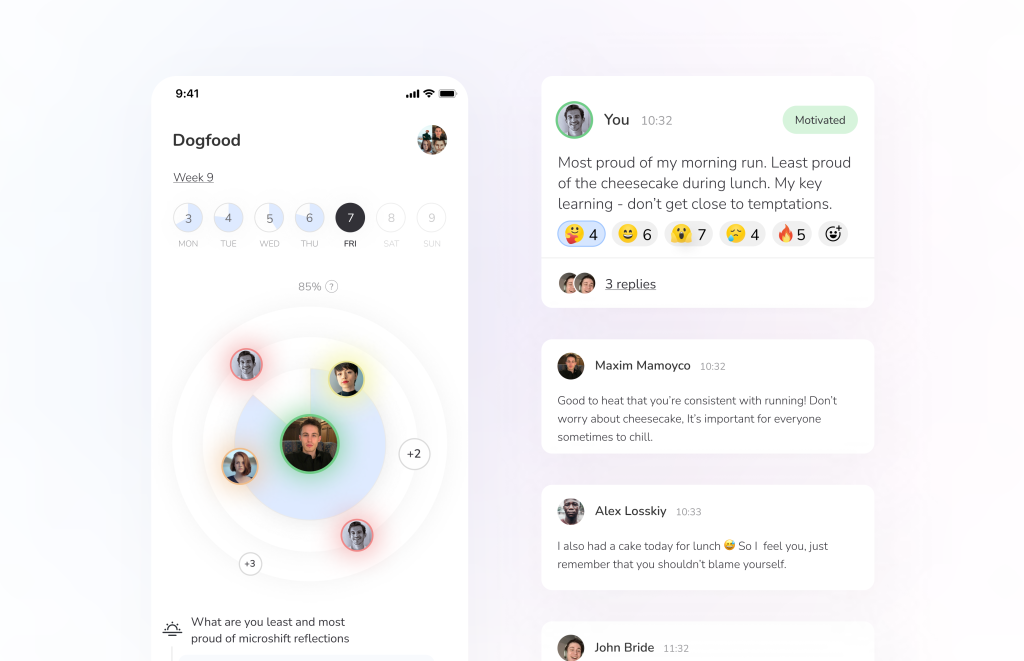
Learn how we’ve built mental health platform for Swedish startup
Benefits of telemedicine for doctors: healthcare providers expand their practices and can reach more patients beyond their local area.
3. Reduced healthcare expenses
Telemedicine benefits for patients include significantly decreased healthcare costs. Healthcare software development of its apps has allowed providers to streamline operations, cut overhead costs related to physical facilities, and optimize resource allocation.
Patients also experience cost savings, avoiding expenses on transportation, parking, and, in some cases, accommodation when seeking medical care away from home. Additionally, telemedicine often results in quicker diagnoses and treatments, preventing the progression of illnesses and further reducing healthcare expenses.
4. Enhanced patient engagement
More of the advantages of telemedicine. Effective doctor-patient communication is crucial for quality healthcare, and mobile apps have transformed this aspect by boosting patient engagement. Through these apps, patients can easily access their medical records, test results, and treatment plans.
Healthcare app development has facilitated the integration of features such as appointment reminders and medication tracking. Note: Such features can help patients stay engaged in managing their health, leading to better treatment adherence and improved health outcomes.
However, this is only the case if you are fulfilling point 1 of this article. For instance, below is the interface that is most familiar to the target audience of the mental health app we developed. This is identified through User Tests.
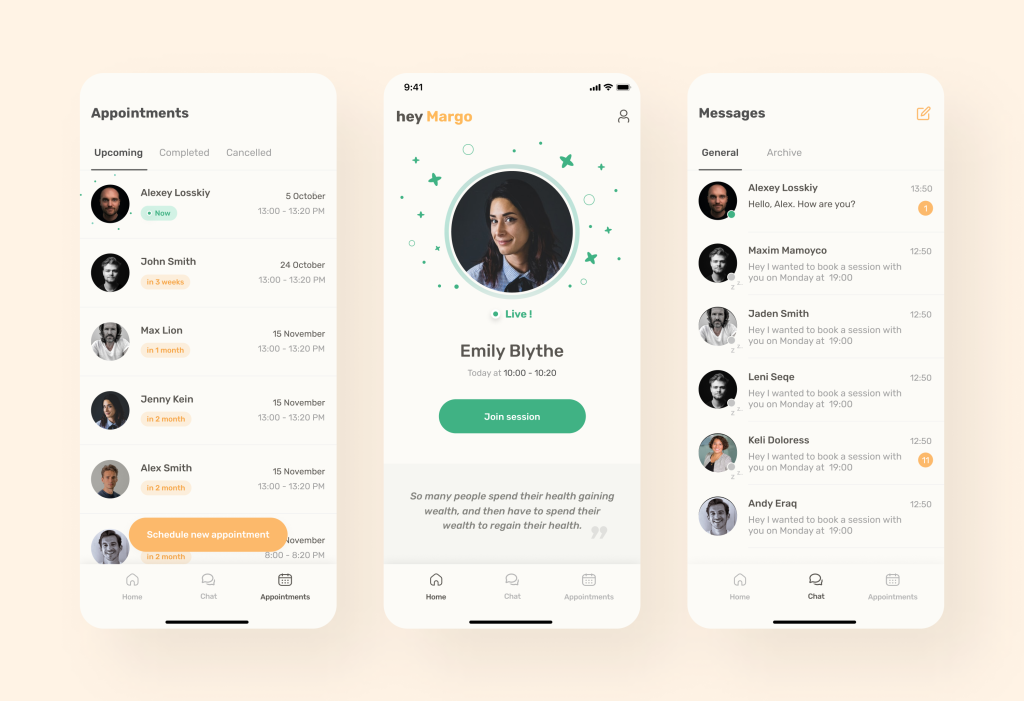
5. Advanced health monitoring
Benefits of telemedicine for doctors: mobile apps have enabled healthcare providers to remotely monitor patients’ health conditions. Patients can use connected devices to measure vital signs like blood pressure, glucose levels, or heart rate and share this data with their healthcare providers through the app.
Real-time data empowers doctors to make informed decisions about a patient’s treatment plan promptly. It also allows for early intervention in case of deteriorating health, reducing the risk of complications.
But telemedicine has benefits and disadvantages. Therefore, it is important to remember that a significant drawback is unfamiliarity and lack of accessibility for various population groups.
The key here is to make the statistics accessible from a UI and UX perspective. To achieve this, represent data from the wearable device in a clear format: utilize meaningful labels, icons, and visualizations that resonate with users. Avoid clutter and prioritize essential data to prevent overwhelming users.
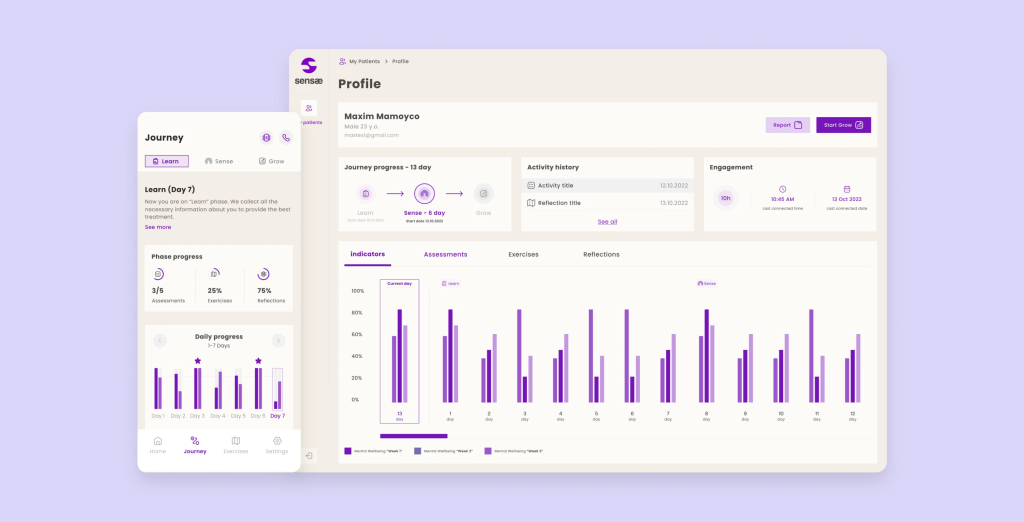
Learn how we’ve built AI health platform for Danish company
6. Privacy and security assurance
Patient data privacy and security are paramount in healthcare, and healthcare software development ensures that these apps incorporate robust security measures. Standard practices include data encryption, secure user authentication, and compliance with healthcare regulations such as HIPAA (Health Insurance Portability and Accountability Act).
Patients can trust that their sensitive medical information is safeguarded when using telemedicine apps, fostering trust between them and their healthcare providers.
How to create a Safe & Compliant Telehealth App
7. Time-efficient healthcare
Time is a valuable resource for both doctors and patients, and telemedicine apps contribute to significant time savings for everyone involved. Patients can avoid long commutes and crowded waiting rooms, while doctors can efficiently manage their schedules, reducing idle time between appointments.
This increased time efficiency benefits healthcare providers, allowing them to see more patients in a day and allocate more time to complex cases. For patients, it means shorter waiting periods for appointments and quicker access to care.
8. Seamless continuity of care
Benefits of telemedicine for patients are obvious here: healthcare is an ongoing process, and the continuity of care is crucial for managing chronic conditions or following up on treatments. Telemedicine apps facilitate continuous communication between patients and healthcare providers. Patients can easily schedule follow-up appointments, ask questions, and provide updates on their health status. We have left a detailed example below the link.

How we create an app for EMDR therapy
This ongoing connection ensures that patients receive consistent care and support, contributing to better long-term outcomes.
Conclusion
These were telemedicine benefits. And we give recommendations for future development:
1. Continuous user education: implement ongoing user education initiatives for seamless onboarding.
2. Innovative engagement strategies: develop strategies to sustain user interest, such as gamification or regular updates.
3. Enhanced interoperability: focus on seamless integration with broader healthcare ecosystems for comprehensive patient care.
4. Technological accessibility: prioritize inclusive design to overcome technical barriers and enhance accessibility.
5. Cybersecurity advancements: stay at the forefront of cybersecurity measures to maintain patient trust and data security.
By the way, here we wrote about the telehealth app development & implementation in the guide format

And we hope this article was useful for you!
Who we are? We are a digital health product studio, who transforms healthcare digital experiences and sets new standards for delivering digital healthcare in a way that positively impacts people’s lives.
We assist healthcare startups in designing and developing digital products, while also helping healthcare organizations undergo transformative changes.
If you are interested about our experience check our portfolio with case studies by the link or you can read more about us here.
And write to us now on m@nozomihealth.com and we will discuss how we can help ensure that your product brings real benefits